|
Health Watch
Benefits of LASIK surgery
Ruwanthi Abeyakoon
Spectacles or contact lenses are vision correction devices
mechanically adjusted to human eyes. These very devices which are of
immense help in life at times hinder our daily activities. Losing your
glasses or contact lenses is one such worry. Spectacles may also get in
the way when you play any sport or enjoy any outdoor activity or you
might just not feel confident on how you look in glasses. The Nawaloka
Hospital's LASIK centre offers a solution for this issue with the
introduction of latest state of the art technology in LASIK Surgery.
 “LASIK
is a laser surgery that reshapes the middle layers of the cornea so that
light rays entering the eye are correctly focused (refracted) on the
retina, the layer of tissue at the back of the eye responsible for
vision. LASIK vision correction is a permanent change and reduces the
need to wear glasses or contact lenses,” said Dr. C.A.B Makuloluwa,
Consultant Eye Surgeon. “LASIK
is a laser surgery that reshapes the middle layers of the cornea so that
light rays entering the eye are correctly focused (refracted) on the
retina, the layer of tissue at the back of the eye responsible for
vision. LASIK vision correction is a permanent change and reduces the
need to wear glasses or contact lenses,” said Dr. C.A.B Makuloluwa,
Consultant Eye Surgeon.
LASIK is the abbreviation for “Laser assisted In-situkeratomileusis”.
Despite the long name, this surgery is a very short, easy and relatively
painless procedure. “LASIK eye surgery can correct nearsightedness
(myopia), farsightedness (hyperopia) and astigmatism, which are usually
corrected with glasses or contact lenses. Certain people with presbyopia
(normal age-related loss of near vision), also may benefit from LASIK
eye surgery, although there are limitations,” Dr. Makuloluwa said.
LASIK improves vision without having to rely on glasses or contacts.
The procedure offers a faster recovery time for best vision and less
discomfort than similar laser surgeries. “To under go this surgery one
should be a suitable candidate. One should possess generally healthy
eyes and cornea, free from diseases and have had stable refractive
errors for at least one year. This surgery is not performed on pregnant
or nursing mothers,” Dr. Makuloluwa said.
“Some people are better candidates than others therefore it is
important to consult your Eye Surgeon to discuss the realistic benefits
which differ from patient to patient,” he added.
Dr. Makuloluwa said that there are three parts to the procedure. “The
eyelids will be kept open by a device called a speculum, while the
patient is requested to maintain eye fixation on a red light during the
procedure. A thin flap of corneal tissue is peeled off with one end of
it still attached to the cornea which is called a flap. It is similar to
a door being opened,” he said.
“The cornea is then reshaped to individual requirement by laser. The
cornea flap is placed back on the cornea (like a door being closed)
within five minutes the flap adheres to its original position without
the use of stitches. The procedure is performed on an “outpatient” on
the day of the surgery. Anesthetic eye drops are administered to numb
the eye for painless surgery.
The overall procedure takes only a few minutes to perform,” Dr.
Makuloluwa added.
This method has been in operation for over 25 years.
Epilepsy ‘is a global health problem’
Epilepsy is twice as common in low and middle-income countries as it
is in the developed world, according to an international team of
researchers.
|
Epilepsy can develop after an infection or damage to the
brain |
They say the higher incidence is linked to increased risk factors,
including head injuries and infections such as pork tapeworm and river
blindness.
And more than 60% of sufferers in those countries receive no
appropriate treatment, they say in the Lancet.
A Lancet editorial said epilepsy had to be a global health priority.
Epilepsy is a condition in which disturbances to the brain's normal
electrical activity cause recurring seizures or brief episodes of
altered consciousness.
There are about 40 different types. Epilepsy is not a mental illness,
but can develop after injury or damage to the brain.
About 85% of the global burden of epilepsy occurs in low and
middle-income countries.
‘Bewitched’
Writing in the Lancet, researchers led by Prof Charles Newton, of the
University of Oxford, say the death rate in developing countries is much
higher than in developed ones - and that the reason for this is likely
to be a failure to treat people with the condition.
Continue reading the main story
“Start Quote
It is time for all governments to take epilepsy more seriously”
Prof Newton said: “The burden of epilepsy in these regions is at
least double that found in high-income countries, and sadly, adequate
facilities for diagnosis, treatment and ongoing management of epilepsy
are virtually non-existent in many of the world's poorest regions.”
He added: “Many people with epilepsy or their families do not even
know that they have a disorder that can be controlled with biomedical
treatment, so it is vitally important that awareness is raised and
medical care improved in these regions.”
Medications are available - but there can be problems distributing
them, especially to remote areas.
The researchers say there are low-cost ways of improving the
situation and of reducing the stigma often faced by people with epilepsy
and their families - such as working with traditional healers and
awareness campaigns to increase understanding of the condition.
In some countries, traditional beliefs about the causes of the
condition, including bewitchment, spiritual causes and curses, lead to
stigma and increase the chance that a person with epilepsy will not get
the treatment they need.
A Lancet editorial adds: “Given the prevalence of epilepsy globally,
it should be included as a priority on the public health agenda, and
access to treatment should be greatly improved in developing countries.
“It is time for all governments to take epilepsy more seriously.”
BBC
IQ linked to levels of happiness
People with lower intelligence are more likely to be unhappy than
their brighter colleagues, according to UK researchers.
Their study of 6,870 people showed low intelligence was often linked
with lower income and poor mental health, which contributed to
unhappiness.
|

A unhappy person |
The researchers are calling for more help and support to be targeted
at people with lower IQs.
Their findings were published in the journal Psychological Medicine.
The researchers, at University College London, analysed data from the
Adult Psychiatric Morbity Survey in England. One of the questions was:
“Taking all things together, how would you say you were these days -
very happy, fairly happy or not too happy?” People's verbal IQ was also
assessed.
The highest proportion saying they were “very happy” was found in
people with an IQ between 120 and 129 - 43% said they were very happy.
However, the highest proportion saying “not too happy” - 12% - was
found in people with an IQ between 70 and 79.
Dr Angela Hassiotis said: “People in the lower end of the normal
spectrum are more likely to consider themselves not happy.”
The study said lower intelligence was linked to lower income, worse
health and needing help with daily life, such as shopping or housework -
all of which contributed to unhappiness.
Dr Hassiotis said: “There is some evidence that long term intensive
strategies directed at young children from socially deprived backgrounds
can have a positive impact not only on IQ, but also on wellbeing and
life opportunities.
“Such interventions are likely to be costly, but the initial costs
may be offset by future benefits such as a reduced reliance on state
benefits and better mental and physical health.” Dr Jonathan Campion, a
consultant psychiatrist and director of public mental health at the
South London and Maudsley NHS Foundation Trust, said: “The study
suggests that higher IQ appears to be associated with improved
wellbeing, but that this relationship between IQ and wellbeing is partly
due to higher IQ being linked with better income, health and less mental
illness.” He added that the study was particularly helpful as it
identified some of the factors that mediate the association between IQ
and happiness, as well as highlighting interventions to prevent lower IQ
leading to greater unhappiness.
BBC
Hi-tech radiotherapy ‘not only answer’
Richard Evans CEO of the Society and College of Radiographers
Radiotherapy has wrongly been “in the shadows” of cancer drugs and
chemotherapy, say those who use it to treat patients.
In this week's Scrubbing Up, Richard Evans, CEO of the Society and
College of Radiographers, says this is beginning to change - but that
there has been too much focus on one hi-tech version, which won't be
right for all.
Amongst the radiotherapy community, there has long been the view that
the pharmaceutical companies are enviably effective in publicising and
marketing their cancer drugs, even those with marginal benefit.
|
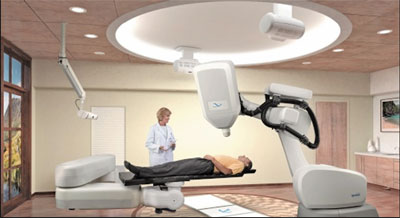
A patient undergoing radiotherapy treatment |
There is also concern that this has had a restraining effect on the
ability of radiotherapy to achieve the prominence it deserves, both
within the public perception and in terms of political focus.
However, all of this seems to have changed with the emergence of new
technology known as Sterotactic Ablative Radiotherapy (SABR) and of one
specific device to deliver it: the Cyberknife.
‘Righteous indignation’
The goal of all radiotherapy is to deliver a lethal dose of radiation
to the cancer cells, whilst minimising damage to normal, healthy body
tissues.
What SABR can do is to achieve this in some parts of the body that
previously would have presented too much risk to those healthy organs.
Hard to treat cancers can, in some cases, now be effectively treated.
There are several excellent machines capable of giving SABR
treatments.
The particular success of the Cyberknife is that it's promoters have
overcome the constraints of poor perception of radiotherapy and have
succeeded in making the product known to politicians, the media and
public alike.
This has been so successfully done that the Cyberknife phenomenon is
beginning to take on characteristics similar to a pharmaceutical
campaign.
Continue reading the main story
No one believes that you need to have a heart surgeon to operate on
your bunions”
There have been on-line petitions demanding access to Cyberknife for
all cancer patients; politicians apparently believing that they have a
duty to see Cyberknife installed in their local cancer centre; the media
carrying pages of righteous indignation over the lack of “life-saving
Cyberknife treatment” and consequently people fighting cancer and their
families caught up in the frenzy.
Just as radiotherapy receives something approaching appropriate
publicity, there are real worries that it is the “wrong type” of
publicity.
The fact is that, despite its brilliance, Cyberknife is simply not
the best machine to treat the vast majority of people that need
radiotherapy.
No one believes that you need to have a heart surgeon to operate on
your bunions.
In the same way, SABR (including Cyberknife) is best employed in
specialist centres where there is appropriate expertise and support.
‘Genuine danger’
Of course, every patient that may benefit from SABR should be able to
receive it. However, this does not mean that there has to be a grossly
under-used expensive Cyberknife in every radiotherapy centre. With many
radiotherapy machines reaching the end of their useful lives, it has to
be folly to believe that replacement should be with anything other than
the best equipment to treat the largest numbers of people. It has been
estimated that, in the UK, up to two people in every six who need
radiotherapy still do not receive it.
There is a genuine danger that the focus on Cyberknife is causing a
distraction that may slow the progress that is being made to close the
gap.
Nevertheless, it is not too late to see the enthusiasm in Cyberknife
as an opportunity rather than a threat.
After all, it should not be too far-fetched to believe that everyone
really wants the same things.
Clinicians, patients, policy makers, carers, equipment manufacturers,
pressure groups, charities, councillors. All want to see people with
cancer receive the best possible care.
We must be able to agree what is best practice, separate from
commercial interest.
This means ensuring wide access to radiotherapy for all those
currently missing out and SABR for those who would benefit. It does not
mean SABR in every radiotherapy department.
BBC
|

A scene from the health camp |
The fourth Annual Health Camp of Janasarana Foundation
The annual Health Camp of Janasarana Foundation was held at
Moneragala Vipulananda Tamil Maha Vidyalaya recently. This year it was
organized as a joint project with the office of the Deputy Inspector
General of Police and 13 Police Divisions in the Moneragala District.
More than 4000 people were examined and given free medications. The
Health Camp had General, Paediatric, Maternity sections and also Blood
Sugar tests, Eye Screening for cataract and Cancer Detection Tests were
done free. Dr. Soma Edirisinghe, Founder/Chairperson of Janasarana
Foundation and Mr. M. R. Latheef, DIG of Moneragala were also present at
this event.
Insomnia: relax… and stop worrying about lack of sleep
What is the solution to the torture of insomnia? Drugs? Therapy? Or
are different sleep patterns natural? A new book investigates.
Every night, about a third of adults have problems falling or staying
asleep that aren't related to a persistent sleep disorder. As they lie
in bed, many are caught in the classic paradox of insomnia: wanting
sleep so badly that they can't get it. “The condition of sleep is
profoundly contradictory,” notes Emily Martin, a professor at New York
University who has studied insomnia. “It is a precious good … but it is
a good like none other, because to obtain it one must seemingly give up
the imperative to have it.”
For doctors, insomnia presents a chicken or egg problem. Is
sleeplessness a result of another condition such as depression, or is
the insomnia the root of the other problem? One report by the US
National Institute of Mental Health found that depression rates were 40
times higher for patients with insomnia than those without sleep
problems. Mental health experts increasingly view depression or anxiety
as an effect, rather than a cause, of insomnia. Taking care of insomnia
may therefore calm other aspects of a patient's life.
And yet insomnia is a unique and difficult condition to treat because
it is self-inflicted.
The cause is often the brain's refusal to give up its unequalled
ability to think about itself, a metaphenomenon that Harvard professor
Daniel M Wegner has called “the ironic process of mental control”.
To illustrate this concept, imagine someone telling you that you will
be judged on how quickly you can relax. Your initial reaction most
likely is to tighten up. After he posed that challenge to research
subjects, Wegner found that the average person becomes anxious as his or
her mind constantly monitors its progress toward its goal, caught up in
the second-by-second process of self-assessment.
In the same way, sleep becomes more elusive as a person's sleep needs
become more urgent. This problem compounds itself each night, leading to
a state of chronic insomnia.
Treating insomnia isn't easy. Part of the reason is that science, as
a whole, has a fuzzy definition of what constitutes the disorder. One
night of bad sleep because of a blaring car alarm or an upcoming
stressful day at work doesn't classify as insomnia. Instead, it is
generally thought of as a string of otherwise peaceful nights during
which a patient can't fall asleep when he or she wants to.
The US National Institutes of Health (NIH) identifies the condition
as “difficulty getting or staying asleep, or having non-refreshing sleep
for at least one month”.
The classic form has no known cause, yet is widespread. About one in
10 people in the US suffer from it during their lifetime.
There is no medical test that proves whether someone is suffering
from a temporary bout of sleepless nights or a more serious disorder.
Some patients go to sleep labs and undergo tests to rule out
conditions such as sleep apnea, but knowing what they don't have offers
little help in treating what they do.
Instead, doctors rely on self-reports from patients, which can be
maddeningly vague, a result of the difficulty that we have with
accurately noting how many hours we truly spent sleeping on any given
night. Patients who have spent a night in a sleep lab, for instance,
often complain that it took them more than an hour to fall asleep when a
chart of their brain waves shows they were asleep within 10 minutes.
Problems of self-reporting aren't limited to judging how long it took
to get to sleep. Some patients wake up in labs claiming that they didn't
sleep at all during the night, despite hours of video and brain wave
evidence to the contrary.
Stressed at work? Look out for your heart
People who have highly demanding jobs and little freedom to make
decisions are 23 percent more likely to have a heart attack compared
with their less stressed out colleagues, according to research published
on Friday. But lighting up a cigarette or remaining chained to your desk
rather than getting out to do some exercise is far more damaging for
your heart health, researchers said.
A study of nearly 200,000 people from seven European countries found
around 3.4 percent of heart attacks can be attributed to job strain - a
significant proportion, but far less than the 36 percent attributable to
smoking and 12 percent put down to lack of exercise.
For the study, which was published online in The Lancet medical
journal, researchers analyzed job strain in employees who had no
previous coronary heart disease (CHD).
Participants completed questionnaires about their job demands,
workload, the level of time-pressure demands and their freedom to make
decisions.
www.healthnews.com |





