Health Watch
IOL VIP system for Macular Degeneration
The IOL Vip system is a hugely exciting breakthrough that has the
potential to offer hope of restoring some of the vision lost to
conditions affecting the central macular region of the retina. The name
IOL Vip stands for intraculor lens for visually impaired people.
Conditions for which the IOL Vip system may be effective include the
following:
* Dry age related macular degeneration (Dry AMD)
* Stable, inactive or previously treated Wet (exudative) age related
macular degeneration (Wet AMD)

* Myopic (short sighted) macular degeneration
* Macular holes
* Inherited macular diseases such as Best’s and Stargardt’s dystrophy
The IOL Vip system has been developed by low vision specialists and
eye surgeons in order to enhance macular function in patients with
macular disease. Thus frequently allowing for an improvement of a
patient’s central vision.
In the IOL Vip procedure, two small lenses are inserted into the eye.
These two lenses work in two ways;
Acting in combination these two lenses act like a miniature
telescope, slightly magnifying the image at the macula.
The lenses can be rotationally aligned in such a way as to divert the
image falling onto the macula away from the most damaged part of the
macula (often the very central part) and towards a less damaged area of
the macula/retina.
Using these two effects the IOL Vip system has demonstrated some
impressive results. In a recent peer reviewed publication involving a
series of thirty five patients, all patients in this group experienced
vision improvement.
The potential improvement in vision can be tested using a special
simulator. The simulator allows a direct demonstration of the effect of
the IOL Vip system so patients can experience the possible improvement
before the operation. Patients can also be helped to learn to use the
new vision with the aid of some simple exercises.
The procedure itself is akin to cataract surgery but using two
separate lens implants instead of one. Typically a procedure will take
around 20-30 minutes and can often be performed under simple eyedrop
anaesthesia. Post operative care is similar to that received in cataract
surgery. Many patients will only require one eye to be operated although
for some best results will be achieved with treatment to both eyes. In
these situations there will normally be a short period of around 2-4
weeks between first and second operation or both eyes can be treated on
the same day.
Age related macular degeneration
Age-Related Macular Degeneration (ARMD) causes a gradually loss of
central vision, but not peripheral vision. Central vision is needed for
reading, driving, recognising faces and doing detailed work. The decline
to severe loss of vision can vary from months to years - depending on
the type the severity of ARMD. Visual loss caused by ARMD cannot
normally be reversed. However, in some cases, treatment may halt or
delay the progression of visual loss.
Understanding the back of the eye
When you look at an object, light from the object passes through the
cornea, then the lens, and then hits the retina at the back of the eye.
The retina is basically made up of two layers. There is an inner
layer of ‘seeing cells’ called rods and cones. These cells react to
light and send electrical signals down tiny nerve fibres (which collect
into the optic nerve) to the brain.
The outer layer - the retinal pigment epithelium - is a layer of
cells behind the rods and cones. These cells help to nourish and support
the rods and cones. They
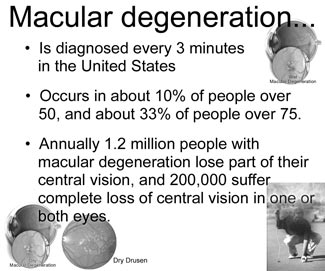 pass nutrients from the blood vessels in the choroid to the rods and cones. They also take waste materials from the
rods and cones to the blood vessels in the choroid. pass nutrients from the blood vessels in the choroid to the rods and cones. They also take waste materials from the
rods and cones to the blood vessels in the choroid.
* The cone cells (‘cones’) deal with colour vision.
* The rod cells (‘rods’) enable you to see shades of grey.
The macula is a small but vital area of the retina at the back of
your eye. It is about 5 mm in diameter. The very centre of the macula is
called the fovea. The macula is the part of the retina that is the most
densely packed with ‘seeing cells’ - especially cones.
The choroid is a layer of tissue behind the retina which contains
many tiny blood vessels. These help to take oxygen and nutrients to the
retina.
Bruch’s membrane is a thin membrane which helps to form a barrier
between the choroid and the delicate retina.
The sclera is the outer thick white layer of the eye.
When you look at an object, the light from the object focuses on the
macula. You need a healthy macula for detailed central vision such as
when reading, writing, driving and recognising faces. The rest of the
retina is used for peripheral vision - the ‘side’ vision which is not
focused. Therefore, without a macula you can still see enough to get
about, be aware of objects people, and be independent. However, the loss
of central vision will severely affect normal sight.
What is age-related macular degeneration (ARMD)?
Age-Related Macular Degeneration (ARMD) is a condition that occurs
when cells in the macula degenerate. That is, they become damaged and
die. Damage to the macula affects your central vision which is needed
for reading, writing, driving, recognising people’s faces and doing
other fine tasks. There are two types - ‘dry’ and ‘wet’ ARMD - described
below.
Who gets age-related macular degeneration?
ARMD is the most common form of macular degeneration and develops in
older people. (There are other rare types of macular degeneration which
occur in younger people). ARMD can affect anyone. It is the most common
cause of severe sight problems (‘visual impairment’) in the UK. It
becomes more common with increasing age. If you develop ARMD in one eye,
you have a high chance that it will also develop in the other eye.
About 1 in 100 people aged 65-75, and about 1 in 8 people aged over
85 have ARMD severe enough to cause serious visual loss. About twice as
many women over the age of 75 have ARMD compared to men of the same age.
The two types of age-related macular degeneration
Dry age-related macular degeneration (dry-ARMD)
This is the most common form and occurs in 9 in 10 cases. In this
type the cells in the retinal pigment epithelium of the macular
gradually become thin (they ‘atrophy’) and degenerate. This layer of
cells is crucial for the function of the rods and cones (the ‘seeing
cells’) which then also degenerate and die. Typically, dry-ARMD is a
very gradual process as the number of cells affected increases. It
usually takes several years for vision to become seriously affected.
Many people with dry-ARMD do not totally lose their reading vision.
Wet age-related macular degeneration (wet-ARMD)
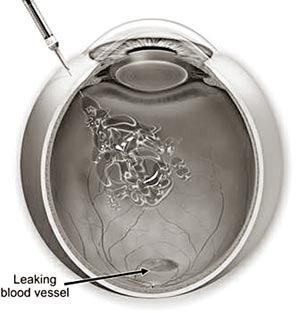
This occurs in about 1 in 10 cases. However, it is likely to cause
severe visual loss over quite a short time - sometimes just months. In
this type of ARMD, in addition to the retinal pigment cells
degenerating, new tiny blood vessels grow from the tiny blood vessels in
the choroid. (This is called ‘choroidal neovascularisation’). The new
vessels break through Bruch’s membrane and into the macular part of the
retina. These vessels are not ‘normal’. They are fragile and tend to
leak blood and fluid. This can damage the rods cones, and cause scarring
in the macula.
What causes age-related macular degeneration?
In people with ARMD the cells of the retinal pigment epithelium do
not work so well with advancing age. They gradually fail to take enough
nutrients to the rods and cones, and do not clear waste materials and
‘by-products’ very well made by the rods and cones. As a result, tiny
abnormal deposits called ‘drusen’ develop under the retina. In time the
retinal pigment cells and their nearby rods cones degenerate, stop
working and die. This is the ‘dry’ type of ARMD.
In some cases, something also triggers new blood vessels to develop
from the choroid to cause the ‘wet’ form of ARMD.
The trigger is not known. It may be that some waste products which
are not cleared from the retinal pigment epithelium may stimulate new
blood vessels to grow in an attempt to clear the waste.
The exact reason why cells of the retinal pigment epithelium stop
working properly in people with ARMD is not known. Certain ‘risk
factors’ increase the risk of developing ARMD. These include:
* Smoking
* Possibly, high blood pressure (inconclusive evidence).
* A family history of ARMD. (ARMD is not a straightforward hereditary
condition. However, your risk of developing ARMD is increased if it
occurs in other family members.)
What are the symptoms of age-related macular degeneration?
* The main early symptom is blurring of central vision despite using
any glasses that you need. In the early stages of the condition you may
notice that:
* You need brighter light to read by.
* Words in a book or newspaper may become blurry.
* Colours appear less bright.
* You have difficulty recognising faces.
* A particular early symptom to look out for with wet-ARMD is visual
distortions. Typically, straight lines appear wavy or crooked. (For
example, the lines on a piece of graph paper, or the lines between tiles
in a bathroom, or the border of any other straight object, etc.)
* A ‘blind spot’ then develops in the middle of your visual field.
This tends to become larger overtime as more and more rods and cones
degenerate in the macula.
ARMD is painless. Symptoms of dry-ARMD tend to take 5-10 years to
become severe. However, severe visual loss due to wet-ARMD can develop
over weeks or months. Therefore, see a doctor or optometrist quickly if
you develop visual loss or visual distortions as treatment may be
possible. Peripheral vision is not affected with ARMD and so it does not
cause total blindness.
If the vision of one eye only is affected, you may not notice any
symptoms as the other good eye often compensates. When both eyes are
affected you are more likely to notice symptoms. Therefore, older people
should have regular eye checks to check on each eye separately for early
ARMD (and to check for other eye conditions such as glaucoma).
How is age-related macular degeneration diagnosed?
If you develop symptoms suggestive of ARMD your doctor or optometrist
will refer you to an eye specialist (ophthalmologist). The specialist
may ask you to look at a special piece of paper with horizontal and
vertical lines. If you find that any section of the lines are missing or
distorted then ARMD is a likely cause of the visual problem. The
ophthalmologist will examine the back of your eye with a magnifier.
There are typical changes that occur with dry-ARMD and wet-ARMD which
can often be seen.
If wet-ARMD is diagnosed or suspected, then a further test called
fluorescein angiography may be done. For this test a dye is injected
into a vein in your arm. Then, by looking into your eyes with a
magnifier and taking pictures with a special camera, the ophthalmologist
can seen where any dye leaks into the macula from the abnormal leaky
blood vessels. This test can give an indication of the extent and
severity of the condition.
Another test called ocular coherence tomography is becoming more
commonly used. This is a non-invasive test that uses special light rays
to ‘scan’ the retina. It can give very detailed information about the
macula and show if the macula is thickened or abnormal. This test is
useful when there is doubt whether ARMD is the wet or dry form. It is
also a useful test to assess the result of any treatment.
Is there any treatment for age-related macular degeneration?
t For the common dry-ARMD- there is no treatment (apart from taking
dietary supplements - see below). However, remember that in this type of
ARMD the visual loss tends to be very gradual, over 5-10 years or so.
t For the less common wet-ARMD - in some cases treatment may halt or
delay the progression of visual loss. Some newer treatments may even be
able to reverse some of the visual loss. Treatments which may be
considered include photodynamic therapy, treatment with drugs and laser
photo-coagulation.
Photodynamic therapy
This is a technique that was developed in the late 1990s. A drug
called verteporfin is injected into a vein on the arm. Within a few
minutes the verteporfin binds to proteins in the newly formed abnormal
blood vessels in the macula. A light at a special wavelength is then
shone into the eye for just over a minute. Verteporfin is a
photosensitive drug. This means that when light is shone at the blood
vessels coated with verteporfin, the verteporfin ‘activates’ and causes
damage and destroys the abnormally growing blood vessels (without
damaging the nearby rods and cones).
Photodynamic therapy is only suitable for some cases. It depends on
exactly where the new blood vessels are growing and their extent. It
does not work in all cases although the success rate in treated people
is high. Success means that the visual loss is prevented from getting
worse - it does not restore any lost vision. Treatment usually needs to
be repeated every few months to continue to suppress newly growing blood
vessels.
Drugs that can treat macular degeneration
In recent years of group of drugs (medicines) called anti-VEGF drugs
have been develop. VEGF stands for ‘VAscular Endothelial Growth Factor.’
This is a chemical that is involved in the formation of new blood
vessels in the macula in people with wet-ARMD. By blocking the action of
this chemical, it helps to prevent the formation of the abnormal blood
vessels that occur in wet-ARMD.
Anti-VEGF drugs include ranibizumab (trade name, Lucentis),
pegaptanib (Macugen) and bevacizumab (Avastin). Others are being
develop. These drugs are injected directly into the vitreous of the eye
by a fine needle and injections are needed every few weeks to keep on
with their effect.
Anti-VEGF drugs are an exciting new development in the treatment of
ARM as they seem to work reasonably well for all types of wet-ARM. For
example, one study of 716 people treated with ranibizumab (published in
the New England Journal of Medicine in October 2006) found that the
treatment slowed visual loss in around 9 in 10 people and improved
vision in about a third.
So, the main aim of treatment with Anti-VEGF drugs is to prevent wet-ARMD
from getting worse. However, it seems that in some cases these drugs may
actually restore some of the vision that has been lost.
It is likely that anti-VEGF drugs will become more widely used. The
National Institute for Health and Clinical Excellence (NICE) in the UK
is currently appraising pegaptanib and ranibizumab to clarify their role
and use in the NHS. Their report is expected in Spring 2008.
Laser photo- coagulation
This is a technique where a fine laser is ‘fired’ at the tiny new
blood vessels that are forming. This destroys the blood vessels which
helps to prevent the condition from getting worse.
However, laser photo-coagulation is only suitable for a small number
of cases. Whether it is suitable depends on exactly where the new blood
vessels are growing as the laser may also damage the rods and cones.
Other treatments
Treatments such as radiation therapy, other drugs and surgery to the
retina are being investigated. For example, a surgical technique where
part of the peripheral retina is grafted into the diseased macular area
is being investigated. The value of these newer treatments is not clear.
The treatment of macular degeneration is an active area of research and
treatment may well improve in the near future.
Diet, dietary supplements and ARMD
A recent large research trial aimed to clarify whether diet and
dietary supplements had a role to play in the treatment of ARMD. It was
called the ‘Age-Related Eye Disease Study’ (AREDS). This showed that in
some cases, high quantities of dietary supplements that contain the
antioxidant vitamins A,C,E, beta-carotene and the minerals zinc and
copper, can help to slow down the progression of ARMD. The study
suggests that people at high risk for developing advanced ARMD should
consider taking these dietary supplements. People at high risk are
defined as people having either:
t intermediate ARMD in one or both eyes (to help prevent ARMD from
getting worse),
OR
t advanced ARMD in one eye, but not the other eye (to help prevent
deterioration in the better eye).
The supplements taken should only be those recommended by your doctor
or eye specialist. This is because some supplements that are marketed to
the general public for ARMD do not contain the correct doses.
Also, there is some concern that the high doses needed may lead to
side effects in some people. For example, beta-carotene has been found
to increase the risk of lung cancer in smokers; vitamin E has been
associated with an increased risk of heart failure in people with
vascular disease or diabetes; zinc may increase your risk of developing
bladder and kidney problems. (So, for example, the supplements are
probably not suitable for current or ex-smokers due to the increased
risk of developing lung cancer).
In short, before taking these high doses of vitamins and minerals,
you should talk with your doctor about the risk of developing advanced
ARMD and whether taking these high dose supplements is right for you.
Research continues to clarify the role of diet and dietary
supplements.
Practical help
When your vision becomes poor, it is common to be referred to a low
vision clinic. Staff at the clinic provide practical help and advice on
how to cope with poor vision. For example, advice about:
l Magnifying lenses, large print books and bright lamps which may
help with reading.
l Gadgets such as talking watches and kitchen gadgets which can help
when vision is limited.
l Being registered as partially sighted or blind. You may then be
entitled to certain benefits.
Further help and information
The Macular Disease Society
Darwin House, 13a Bridge Street, Andover, Hampshire, SP11 6NN
Tel: 0845 241 2041
Web: www.maculardisease.org
|



