|
Health Watch
Food allergies in children! Be alert!
Charmaine Fernando
With the season of merriment and good cheer knocking at your door its
hard not to show your flare for hospitality. Being Sri Lankans, we have
a penchant to go overboard when it comes to treating our guests who drop
by to wish us a Merry Christmas. I have always wondered how the ‘merry’
got attached to the holy bible story of Christmas, but never gathered
enough clues for conviction.
|

Lobster |
Merrymaking has come home to stay. Christmas brings home to us the
sweet scent of pine mingled with the hard to ignore spicy aroma of
irresistible rich foods, baking in every Christian home and hearth. A
wise man insists that Christmas is for children. Next to playing the
merry old Santa on Christmas Eve, filling the sock with enchanting toys
that light up kiddies world we need to pay attention to what the kiddie
might consume during the season. Getting carried away with the glorious
intricacies of enjoyment we may tend to forget the babe, like we all do
at Christmas, losing its very essence.
Talking about food and children against a season of merrymaking and
hospitality have your eyes open and mind alert to the slightest symptom
of food allergies, especially in children. It doesn’t mean you should
loosen your grip on sensitivity to it throughout the year. Food
allergies are more common in children than adults. About seven out of
100 kids have them. Only about three to four out of 100 adults do.
Children often outgrow their food allergies. But if you have a food
allergy as an adult, you will most likely have it for life.
True food allergies are not as common as most people believe and only
affect about two percent of children, although they are more common in
younger children, affecting about five to eight percent of younger
children. Fortunately, younger children will outgrow these food
allergies by the time they are three years old. Now
|

Pineapple |
that’s what I call good news for parents of toddlers who suffer from
allergies.
Symptoms of a food allergy can include wheezing and difficulty in
breathing, itchy skin rashes, including hives, vomiting, diarrhea,
nausea, abdominal pain and swelling around the mouth and in the throat.
These symptoms usually develop fairly quickly after your child ingests
the food he is allergic to, often within minutes to hours. You must note
that nasal symptoms by themselves, such as congestion or a runny nose,
are usually not caused by food allergies.
Symptoms may be mild or very severe, depending on how much of the
food your child ingested and how allergic he is to the food.
A severe reaction can include anaphylaxis, with difficulty in
breathing, swelling in the mouth and throat, decreased blood pressure,
shock and even death. So, be alert, season or no season. The babe should
be in focus at all times.
More common than food allergies are intolerances to certain foods,
which can cause vomiting, diarrhea, spitting up, and skin rashes. An
example of such a reaction occurs in children with lactose intolerance,
which occurs because of a deficiency of the enzyme lactase, which
normally breaks down the sugar lactose. Children without this enzyme or
who have a decreased amount of the enzyme, develop symptoms after
drinking lactose containing food products, such as cow’s milk. However,
because this reaction does not involve the immune system, it is not a
real food allergy.
If you notice that your child develops symptoms after being exposed
to certain foods, then you should avoid those foods. The most common
foods that can cause allergies include: peanuts, tree nuts (walnuts,
pecans, etc. and rarely coconut), fish, shellfish, eggs (especially egg
whites), milk, soy, and wheat. Keeping a diary for a few weeks and
recording what foods your child has been eating, especially new foods,
and when he develops symptoms may help figure out what he is allergic
to. Finding out the root cause is crucial.
|

People are allergic to Peanuts |
Once you determine what your child is allergic to, it is important to
learn to read food labels because the food your child is allergic to may
be an ingredient of many other foods.
You should also avoid eating foods that may have been prepared using
equipment that was also used to prepare the types of food that your
child is allergic to.
When trying to determine what your child is allergic to, parents
often incorrectly assume that if he has eaten a food before and not had
problems, then he probably is not allergic to that food.
They usually only suspect new foods as being able to cause a food
allergy. However, it is important to keep in mind that it takes time for
the immune system to build up a reaction against something that the body
is allergic to. It may take days, weeks, months or even years to build
up enough of a response to cause noticeable symptoms.
So your child may be allergic to a food even if he has eaten it many
times before without problems. In addition to avoiding what you think
your child may be allergic to, children with more severe reactions
should be evaluated by their Pediatrician or an allergist.
Testing may be done, either skin testing or RAST, a blood test to
check for antibodies against certain things your child may be allergic
to, and see if specific food allergies can be found. In addition, your
child should wear a medical alert bracelet to notify others of his
allergy.
Now you know how important it is to have ‘the babe’ in focus
especially at Christmas! Fill your heart instead of the sock, with
goodness. Have a spirited season!
Important Reminders to Parents
While children often outgrow their food allergies, if your child had
a severe reaction to a food, then you should talk with your Pediatrician
or allergist before reintroducing the food.
Talk with and educate other family members and caregivers about your
child’s food allergies. Most people do not understand how serious food
allergies can be, and may think it is all right to give just a small
amount of a food that your child is allergic to.
Educate your child about his allergy, so that he can learn to avoid
foods that he is allergic to.
|

Even junk food |
If your child does not improve with these interventions or if he has
had a severe allergic reaction, then you should consider having him see
an allergy specialist for testing to figure out what foods he is
allergic to and to possibly start allergy injections.
Children with severe allergic reactions or anaphylaxis should wear a
medical alert bracelet to notify others of his condition and should
carry an epinephrine autoinjector (such as the EpiPen JR) to ensure
rapid treatment during an allergic reaction.
Most importantly, learn to read food labels and look for ingredients
that your child may be allergic to and practice strict avoidance of
those foods. If you don’t know what an ingredient is, then call the
manufacturer before giving it to your child to be safe.
Common Food Allergies
A food allergy is an adverse immune response to a food protein. Food
allergy is distinct from other adverse responses to food, such as food
intolerance, pharmacological reactions, and toxin-mediated reactions.
The food protein triggering the allergic response is termed a food
allergen. It is estimated that up to 12 million Americans have food
allergies and the prevalence is rising. Six to eight percent of children
under the age of three have food allergies and nearly four percent of
adults have them.
Food allergies cause roughly 30,000 emergency room visits and 100 to
200 deaths per year in the US. The most common food allergies in adults
are shellfish, peanuts tree nuts, fish and eggs and the most common food
allergies in children are milk, eggs, peanuts, and tree nuts.
Treatment consists of either desensitization or avoidance, in which
the allergic person avoids all forms of contact with the food to which
they are allergic. People diagnosed with a food allergy may carry an
auto injector of epinephrine such as an EpiPen or Twinject, wear some
form of medical alert jewellery or develop an emergency action plan, in
accordance with their doctor.
The most common food allergies are
many but the following top the list.
|

Prawns |
1. Dairy allergy
2. Egg allergy
3. Peanut allergy
4. Tree nut allergy
5. Seafood allergy
6. Shellfish allergy
7. Soy allergy
8. Wheat allergy
These are often referred to as ‘the big eight’. They account for over
90 percent of the food allergies.
The top allergens vary somewhat from country to country but milk,
eggs, peanuts, tree nuts, fish, shellfish, soy, wheat and sesame tend to
be in the top 10 in many countries. Allergies to seeds, especially
sesame seem to be increasing in many countries.
Flu Pandemics:
Be alert for H1N1 pandemic
Dr. Sarath Tennakoon
The smallest known infective agents are the viruses, human beings,
animals, plants and bacteria are susceptible to infection by appropriate
viruses. The small size, the genome (contains only one kind of nucleic
acid) and inert metabolism (viruses have no metabolic activity outside
susceptible host cells and these are intracellular parasites) are the
three main properties of viruses.
|
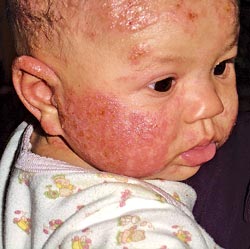
Baby with an allergic reaction |
Viruses can effect the host cell in four ways. If the infection is
lethal the cell gets killed (cell death). The cell may get transformed
to one with properties of a cancer cell and continue to proliferate
haphazardly. The virus could also remain hidden inactive state without
producing obvious ill effects (latent infection).
Some viruses have protein in their outer coats that get stuck to red
blood cells of the host and make them sticky (haemadsorption).
Viruses are important as they cause human disease especially among
children. But most viral infections are mild and the patient makes a
complete recovery. However they can cause severe disease in an unusually
susceptible patient and even cause death. The response of the host to
virus infection is twofold.
The body has a non-specific defence mechanism consisting of barriers
to infection. These are the skin, the respiratory tract, the
gastrointestinal tract, the urinary tract, conjunctiva, the white blood
cells of the blood. The specific immunological defence responses are of
two types. Firstly the humeral mechanism neutralizes the viruses.
Secondly the cellular response is very important for eliminating virus
infected cells.
Occasionally virus infections may erupt suddenly in the form of huge
waves of epidemics known as pandemics which effect large populations in
several countries. Flue pandemics come in waves and become worse as they
spread. Such pandemics have erupted in 1781, 1847, 1890 and 1918.
In 1918-19 there was a particularly severe and great pandemic that
killed between 20 and 40 million people as it spread around the world
(Greenwood et al, 1992).
In 1933 Sir Christopher Andrews and others isolated influenza a
virus. Continuation of virus studies revealed that epidemic behaviour of
viruses is related to changes in the virus itself.
A phenomenon known as “original antigenics in” was identified. This
means that infection with a current virus type stimulates antibody to
earlier strains. By antibody studies of older people the antigenic
components that were prevalent back to the end of the previous century
were deduced. In 1890 the subtype was H2N2, in 1900 it was H3N8, in 1918
it was H1N1 (Swine like Spanish influenza), in 1957 it was HaN2 (Asian
influenza), in 1968 it was H3N2 (Hong Kong influenza), in 1977 it was
H3N2+H1N1 and in 1990 it was H3N2+H1N1 respectively. The major pandemics
have been associated with antigenic shifts - when the viral H or N or
both have changed (Greenwood et al 1992). The WHO (World Health
Organization) monitors influenza A and B throughout the world to see the
appearance of their variants. It is usually the influenza A virus that
undergoes antigenic shift, and not B and C.
Unlike in 1918 currently there are antiviral drugs and vaccines. In
1918 two waves of virus attack were identified. The first was the mild
attack with few deaths and gave a protective effect to the rest to fight
against the severe attack. On the average there was 70 per cent
protection says Simonson who analysed the 1918 flu (Mackensie 2009).
If the current H1N1 virus follows the same pattern as the 1918 virus,
then the same trend could occur. The problem with antivirals is the
development of resistance of the virus either by mutation or through
swapping genes. The cost is yet another issue. Preparation of vaccines
too is a big and costly issue.
“If production begins in June under the best possible conditions, we
could have 190 million doses by September, jumping to a billion by
October, not nearly enough for the world’s people” (New Scientist,
2009).
There are some population groups who are at special risk. The obese,
children, pregnant mothers, Diabetics, those with immunodefieciency and
chronic disease conditions etc, are at special risk. In 1918 it was
found that the practice of social distancing was very helpful in curbing
the pandemic.
Measures like isolating patients and their contacts, closing schools,
banning large gatherings, closing some business and staggering working
hours to this out rush hour, kept the infection levels low in many
places (New Scientist, 2009).
References
1. Greenwood David et al (1992) Medical Microbiology, Churchill
Livingstone.
2. MacKanzie Debora (2009) New Scientist, 9 May 2009
3. Timbury Morag. C (1994) Medical Virology, Churchill
Livingstones, U.K. |



