Chikungunya hits nation once again
Faiz Marikar
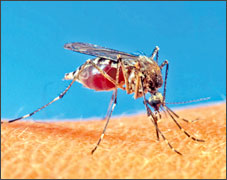
Chikungunya virus (CHIKV) is an alphavirus indigenous to tropical
Africa and Asia, where it is transmitted to humans by the bite of
infected mosquitoes, usually of the genus Aedes. Chikungunya (CHIK)
fever, the disease caused by CHIKV, was first recognized in epidemic
form in East Africa during 1952-1953.
 The
word "chikungunya" is thought to derive from description in local
dialect of the contorted posture of patients afflicted with the severe
joint pain associated with this disease. Because CHIK fever epidemics
are sustained by human-mosquito-human transmission, the epidemic cycle
is similar to those of dengue and urban yellow fever. The
word "chikungunya" is thought to derive from description in local
dialect of the contorted posture of patients afflicted with the severe
joint pain associated with this disease. Because CHIK fever epidemics
are sustained by human-mosquito-human transmission, the epidemic cycle
is similar to those of dengue and urban yellow fever.
Large outbreaks of CHIK fever have been reported recently in Sri
Lanka. In December 2006, CHIK fever cases also have been reported in
capital city Colombo transmitted from India. During 2006, more than kilo
cases of CHIK fever virus were diagnosed virologically.
Clinicians should be alert for additional cases among fever patients,
and public health officials should be alert to evidence of local
transmission of chikungunya virus (CHIKV), introduced through infection
of local mosquitoes by a person with viremia.
Transmission
Aedes aegypti and Aedes albopictus (the Asian tiger mosquito) are the
primary CHIKV vector in Sri Lanka. In Asia, CHIKV epidemics involve a
human-mosquito cycle, with humans serving as the sole vertebrate
amplifying hosts. Most CHIKV epidemics occur during the tropical rainy
season and abate during the dry season.
Human CHIKV infections include a transient, high-titered viremia
(typically detectable during the first 2 days of illness, ranging up to
6 days after illness onset) that is adequate to infect feeding
mosquitoes.
Ae. aegypti and Ae. albopictus are abundant peridomestic species and
aggressive daytime blood-feeders in all tropical and most subtropical
areas of the world, and Ae. albopictus now lives in many part of Sri
Lanka. Early recognition of local transmission followed by prompt,
aggressive vector control and other public health measures might prevent
long-term establishment of the virus in new areas.
Symptoms and prevention methods
Most CHIKV infections are symptomatic. In clinical infections, the
incubation period typically is 2-4 days. Illness is characterized by
sudden onset of fever, headache, malaise, arthralgias or arthritis,
myalgias, and low back pain. Skin rash occurs in approximately half of
cases. Joint symptoms can be severe and involve small and large joints.
Although CHIK fever typically lasts 3-7 days and full recovery is the
usual outcome, certain patients experience persistent joint symptoms for
weeks or months and occasionally years after illness onset. Serious
complications (e.g., neuroinvasive disease) are rare, and fatal cases
have been documented conclusively (very rare). Transplacental CHIKV
transmission and severe congenital CHIKV disease have been described.
CHIKV infection is believed to confer life-long immunity.
Because no specific drug therapy is available, treatment of CHIK
fever is supportive. No licensed CHIKV vaccine exists. Therefore,
prevention recommendations for people who live in outbreak areas in Sri
Lanka should emphasize mosquito repellent and avoidance measures.
Clinical features
In early illness, the clinical features of CHIK fever can be similar
to those of dengue and malaria, especially in patients without joint
symptoms. In both dengue and CHIK fever, rash usually is generalised and
maculopapular, but petechial rashes occur in certain dengue cases.
Additional imported but unrecognised cases likely occurred in this
nation. Clinicians should be aware of possible CHIKV infection in
travelers returning from CHIK-fever endemic or outbreak areas,
particularly if an acute febrile illness with arthralgias or arthritis
occurs.
Suspected cases should be reported promptly to local and state public
health officials and to MOH. Mosquito exposure should be strictly
avoided during the first week of illness to prevent infection of local
mosquitoes.
Diagnostic tests
In Sri Lanka, diagnostic tests for CHIKV infection are available at
Gentech, MRI, and Ragama Medical Faculty. Laboratory diagnosis depends
on antibody-capture IgM ELISA, and plaque-reduction neutralisation tests
of serum. Virus isolation attempts and PCR assays are performed
selectively.
The writer is Senior Lecturer, Department of Biotechnology and
Bioinformatics, Sri Lanka Institute of Information Technology
|

